Most people have experienced Xerosis, or dry skin, at some stage of their life. When it becomes severe, it can affect people, both physically and emotionally. Following a suitable skin care routine that does not exacerbate the condition and provides adequate care and moisture is the key to controlling the symptoms of Xerosis. Understanding the various causes and the relevant solutions aids personalising the routine to enhance its efficacy.
Xerosis – what is it?
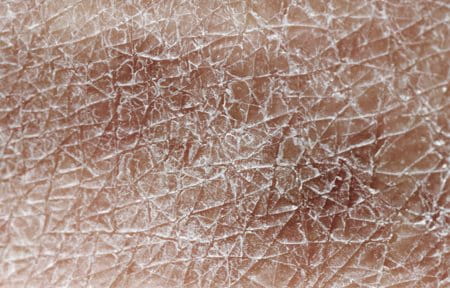
Xerosis is the medical name for dry skin. It comes from Greek; ‘xero’ means ‘dry’, and ‘osis’ means ‘disease’ or ‘medical disorder’. It is caused by a lack of water in the skin, which may be caused by ageing (senile Xerosis) or by underlying diseases like diabetes. The result is dry, rough and tight skin, which can progress to become very rough, and even scaly and flaky.
Attention
Whenever you are unsure about your skin condition it is important to consult your dermatologist for a face-to-face diagnosis. The skin test can also be a helpful tool.

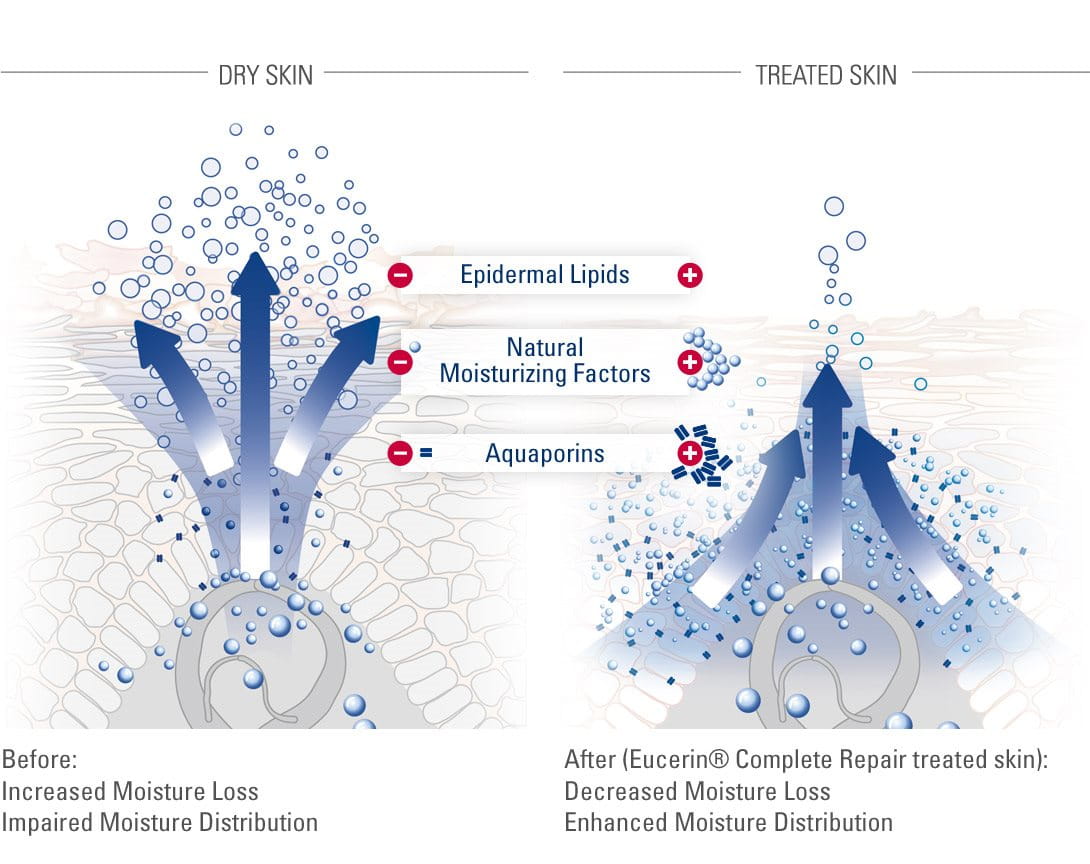
The skin’s ability to regulate hydration, or the concentration of water in the upper layers, is dependent on three key factors, which occur at different depths within the skin:
- In the upper layers of the skin, various hygroscopic molecules, such as urea, lactate, PCA (pyrrolidone carboxylic acid), salts and amino acids, attract and bind large quantities of water.
- Skin´s own barrier lipids (e.g. Ceramide-3) perform the vital function of reducing water loss due to evaporation.
- In the deeper skin layers, skin´s own vital moisture network pass water upwards through Aquaporin channels.
Read more in dry skin in general
This delicate system works well and adapts to the skin’s hydration requirements, maintaining an adequate concentration of water in a changing environment. However, several internal (endogenous) and external (exogenous) factors can disrupt this system, leading to dry skin. The severity of the symptoms depends on the number of compounding factors.
Xerosis – signs and symptoms
Xerosis is a common condition experienced by millions of people, either chronically or acutely. Just as multiple factors support skin hydration, a lack of water within the skin can present in a variety of ways. Most often dry skin will display a couple of these symptoms, while very dry skin commonly has all of these symptoms to some degree:
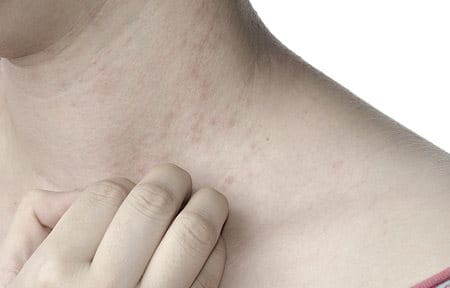
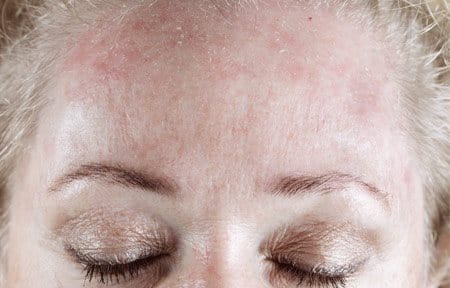
- Tightness is caused by the skin losing its elasticity due to being dehydrated. Skin becomes less flexible when dehydrated, and loses volume when there is a deficiency of water.
- Roughness is also caused by dryness which increases the rate of cell death in the upper skin layers, leaving a thicker layer of dead cells at the skins surface.
- Scaly skin is similar to rough skin, only that the upper skin layer, or stratum corneum, has become dry and inflexible.
- Flakey skin occurs when the scales of dry skin peel off. Sometimes this may only be a fine dust.
- Itching is another result of dryness, and is an impulsive reaction to the discomfort caused by tight, poorly functioning skin.
- Sensitivity is caused by the dry skin being unable to prevent irritants,such as hot water, perfumes and chemicals from penetrating the skin´s surface. However, sensitive skin is not always caused by dryness.
Inflammatory skin conditions such as Atopic Dermatitis and Psoriasis predominantly cause localized areas of xerotic skin. Read more about Psoriasis, Atopic Dermatitis on face or body or about atopic children´s skin on face or body.
Attention
Always seek professional advice for a face-to-face diagnosis if you develop any of these symptoms.
Xerosis – what causes it?
Three key deficiencies in the skin have been shown to contribute to Xerosis:

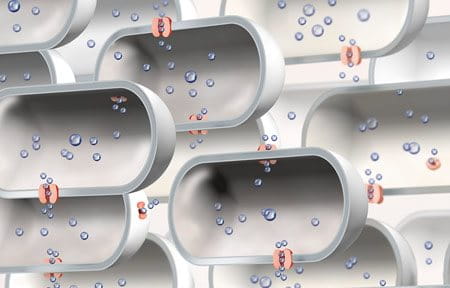
A deficiency in skin barrier lipids
The cells in the horny layer are bound together by epidermal lipids. These lipids are essential for healthy skin: they create its protective barrier and bind in moisture. When lipids are missing, skin can become dry and may feel tight and rough.
A deficiency in natural moisturising factors (NMFs)
The skin also contains several other natural moisturising factors (NMFs) in addition to Urea. These are Lactate, PCA, salts and sugars. Like Urea, these natural moisturising factors, attract moisture towards, and bind moisture into, the stratum corneum, or upper layer of the skin, preventing it from becoming dry, scaly and damaged.
A deficiency in the skin’s own moisture network
Aquaporins are microscopic water channels located in cell membranes that control the water transfer into and out of the cells.
Aquaporins make up a network that conveys moisture through the different epidermal skin layers.
Factors that contribute to dry skin
Several external factors initiate the above physiological changes that may lead to Xerosis:



The skin’s external environment – humidity, cleansing and sunlight
- Dry skin is more common when environmental humidity is low, which occurs in the winter and sometimes during a hot summer.
- Cleansing, especially if frequent, causes the skin’s natural barrier to be destroyed. This is particular true when using harsh cleansers or detergents.
- Sunlight can cause skin dryness as the UV light increases the rate of evaporation from the skin, and, over the longterm, can cause the skin to age prematurely which affects its ability to maintain adequate hydration.
The skin’s internal environment – age, dehydration, diet, medication and disease
- Studies have reported that lipid levels in the stratum corneum are reduced with ageing. This can lead to age-induced dryness.
- A dehydrated body cannot afford to supply water to the skin.
- Diet is important as the vital lipids, NMFs and nutrients are necessary for a healthy skin.
- Certain medications, particularly diuretics, cause the body to become dehydrated, which in turn can lead to Xerosis.
- Skin conditions such as Atopic Dermatitis, Psoriasis and Diabetes include dry skin as a common symptom.
Xerosis – what can be done?
Historically, treatment of Xerosis has been primarily symptomatic, with the aim being the short-term relief of symptoms through the topical application of lipids, mainly vegetable oils, humectants and NMFs, such as urea and lactate. As more is understood about the causes and triggers of Xerosis, clinicians have discovered that a more holistic, enduring approach to treating Xerosis yields superior results. This strategy begins with avoiding, or minimising, the causes and contributing factors of Xerosis, centres on maintaining an adequate skin care routine for face and body of cleansing and moisturising.
Cleansing dry skin

Mild but effective skin cleansing is an essential prerequisite not only for the following application of topical treatments, e.g. in Atopic Dermatitis, but also of facial moisturisers in the care of dry skin conditions. The selection of a well suited skin cleansing product which does not compromise skin barrier function is crucial for the efficacy of a subsequent skin moisturising treatment.
Improving skin hydration
Skin hydration is regulated in many ways, each of which is influenced by many different factors. To effectively treat Xerosis, each factor involved in modulating and maintaining skin hydration should be addressed.


Urea is often deficient in dry skin and therefore a common ingredient in moisturisers. Additional causes of Xerosis are a lack of further natural moisturising factors (NMFs) and skin barrier lipids. Supplying these vital molecules topically can restore the skin’s ability to regulate hydration. Additionally, a novel humectant and conjugate of glycerol and glucose, glyceryl glucoside (GG), has been shown to stimulate the skin´s own moisture network.
When clinically assessed for the treatment of Xerosis in comparison to the lotion base (vehicle) containing Urea, Lactic Acid and Glycerol, these moisturisers containing a range of NMFs, Gluco-glycerol and Ceramide-3 provided superior skin hydration and longer-lasting moisturisation, and therefore represent an advancement in the treatment of Xerosis. Further, both these moisturisers significantly improved skin hydration, skin barrier function, visible dryness, and tactile roughness compared to their vehicles. Skin tolerability was also very good.
In summary, skin care products such as the Eucerin Urea range, formulated with unique combinations of effective skin hydrating agents that address the key deficiencies occurring in Xerosis, provide advanced therapeutic options for the treatment of this skin disease.
Attention
If symptoms change or if you are unsure which treatment suits you best, please seek for dermatologist´s advice.
Avoiding contributing factors
In addition to having a good cleansing and moisturising routine, avoiding factors that contribute to dry skin is important. This will help to reduce the impact of dry skin and the need for treatment:

- Avoid dry air by spending less time outdoors in hot arid or cold weather, and by using a humidifier indoors when the heating is on.
- Reduce the time spent in hot water by having quick lukewarm showers instead of long hot baths.
- Using gloves when washing dishes will help to avoid hot water and strong detergents.
- Wear clothes made of natural materials like cotton and silk that do not irritate the skin. Wool is natural but can irritate atopic skin , and should be avoided in this condition.
- Try to use a clothes detergent without dyes or perfumes, as these can remain on the clothes after washing and might irritate dry skin.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.





